If you need health coverage sign up for a qualifying plan, please click the button below:
The Patient Protection and Affordable Care Act (ACA) became law in early 2010, but its primary requirement that most Americans carry health insurance – the “individual mandate” – is just now taking effect.
To help you, we’ve created a tutorial to walk you through what taxpayers have to do in order to comply with the ACA. We cover all the essential points:
- Who must be insured, and who gets an exemption
- What coverage is required, and what insurance plans provide it
- What the Health Insurance Marketplaces are and what they offer
- The premium credit and other financial assistance to make insurance more affordable
- The penalty for not having coverage
We’ve also created calculators to help you answer what are likely to be some key questions about your insurance coverage:
SOURCE: DrakeHealth
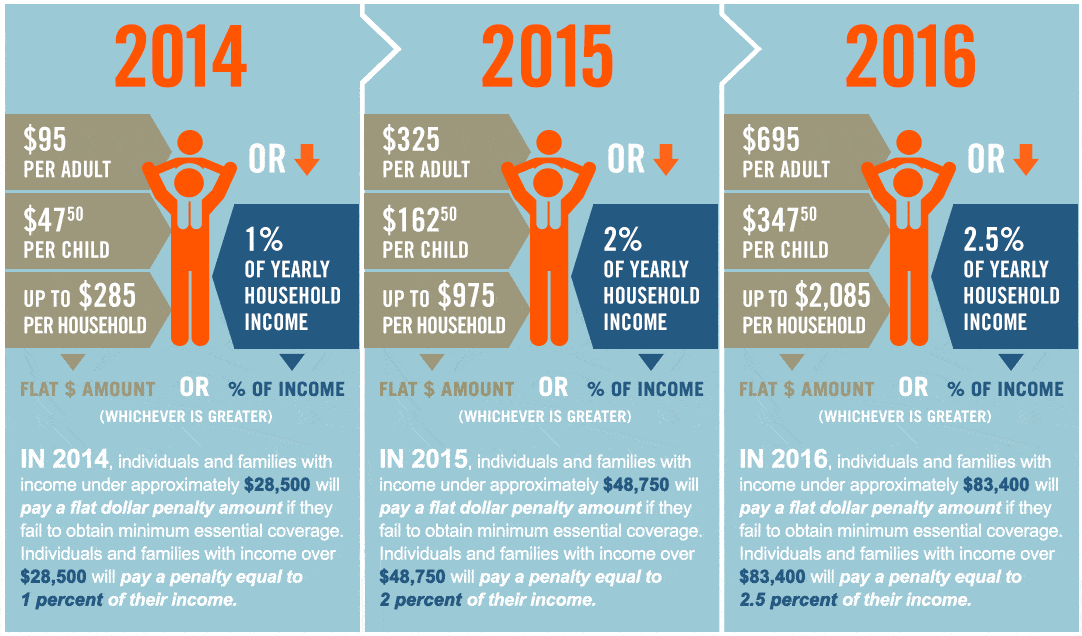
| Exemptions | May only be granted by Marketplace | May be granted by Marketplace or claimed on tax return | May only be claimed on tax return |
|---|---|---|---|
| Coverage is considered unaffordable - The minimum amount you would have paid for employer-sponsored coverage or a bronze level health plan (depending on your circumstances) is more than 8 percent of your actual household income for the year as computed on your tax return. Also see the second hardship listed below, which provides a prospective exemption granted by the Marketplace if the minimum amount you would have paid for coverage is more than 8 percent of your projected household income for the year. |  |
||
| Short coverage gap - You went without coverage for less than three consecutive months during the year. For more information, see question 22 of our questions and answers. |  |
||
| Income below the return filing threshold - Your gross income or your household income is less than your applicable minimum threshold for filing a tax return. Learn more about household income. |  |
||
Citizens living abroad and certain noncitizens - You are:
|
 |
||
| Members of a health care sharing ministry - You are a member of a health care sharing ministry, which is an organization described in section 501(c)(3) whose members share a common set of ethical or religious beliefs and have shared medical expenses in accordance with those beliefs continuously since at least December 31, 1999. |  |
|
|
| Members of Indian Tribes - You are a member of a Federally-recognized Indian tribe, including an Alaska Native Claims Settlement Act (ANCSA) Corporation Shareholder (regional or village), or you were otherwise eligible for services through an Indian health care provider or the Indian Health Service. |  |
||
| Incarceration - You are in a jail, prison, or similar penal institution or correctional facility after the disposition of charges. |  |
||
| Members of certain religious sects - You are a member of a religious sect in existence since December 31, 1950, that is recognized by the Social Security Administration (SSA) as conscientiously opposed to accepting any insurance benefits, including Medicare and Social Security. |  |
||
| Aggregate self-only coverage considered unaffordable - Two or more family members' aggregate cost of self-only employer-sponsored coverage exceeds 8 percent of household income, as does the cost of any available employer-sponsored coverage for the entire family. |  |
||
| Gap in coverage at the beginning of 2014 - You had a coverage gap at the beginning of 2014 but were either enrolled in, or were treated as having enrolled in, coverage through the Marketplace or outside of the Marketplace with an effective date on or before May 1, 2014. See this HHS Question and Answer. |  |
||
| General hardship - You experienced circumstances that prevented you from obtaining coverage under a qualified health plan, including, but not limited to, homelessness, eviction, foreclosure, domestic violence, death of a close family member, and unpaid medical bills. Learn more about the criteria for this exemption. |  |
||
| Coverage considered unaffordable based on projected income - You do not have access to coverage that is considered affordable based on your projected household income. |  |
||
| Determined ineligible for Medicaid in a state that did not expand Medicaid coverage - You are determined ineligible for Medicaid solely because the State in which you live does not participate in Medicaid expansion under the Affordable Care Act. |  |
||
| Resident of a state that did not expand Medicaid - Your household income is below 138 percent of the federal poverty line for your family size and at any time in 2014 you reside in a state that does not participate in Medicaid expansion under the Affordable Care Act. |  |
||
| Unable to renew existing coverage - You were notified that your health insurance policy was not renewable and you consider the other plans available unaffordable. See HHS guidance and HHS Question and Answer for more information.. |  |
||
| Gap in CHIP coverage - You applied for CHIP coverage during the initial open enrollment period and were found eligible for CHIP based on that application but had a coverage gap at the beginning of 2014. See HHS guidance for more information. |  |
||
| AmeriCorps coverage - You are engaged in service in the AmeriCorps State and National, VISTA, or NCCC programs and are covered by short-term duration coverage or self-funded coverage provided by these programs. |  |
||
| Limited benefit Medicaid and TRICARE programs that are not minimum essential coverage - You are enrolled in certain types of Medicaid and TRICARE programs that are not minimum essential coverage (available only in 2014). |  |
||
| Employer coverage with non-calendar plan year beginning in 2013 - You were eligible, but did not purchase, coverage under an employer plan with a plan year that started in 2013 and ended in 2014 (available only in 2014). |  |
